Becoming aware that your partner has no sperm (a condition called azoospermia) can be an overwhelming and emotional experience. You might feel shock, grief, or worry about what this means for your dreams of having a child. If you are facing this situation, it’s important to know you are not alone. Infertility is more common than many realize – roughly 1 in 6 couples worldwide experience difficulty conceiving, and male-factor infertility plays a role in about half of these cases. In fact, complete absence of sperm in the ejaculate (azoospermia) affects about 1% of all men and 10–15% of infertile men. This means thousands of couples are grappling with the same challenge. The good news is that having zero sperm does not mean you cannot have children. With modern fertility treatments and third-party reproduction options, there are multiple paths to parenthood available. This article will explain why azoospermia happens, outline medical and donor options (such as using sperm donors, egg donors, and gestational carriers/surrogates), discuss legal and ethical considerations, and provide guidance on emotional support. Our goal is to offer compassionate, evidence-based information so you can feel empowered and hopeful about building your family despite this diagnosis.
Understanding Azoospermia (Zero Sperm Count)
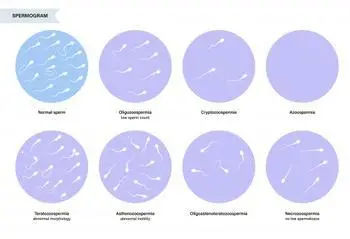
Azoospermia is the medical term for having no measurable sperm in the semen. In other words, when the male partner’s ejaculate is analyzed, no sperm cells are found. It’s important to distinguish this from aspermia, which means no semen at all (for example, in cases of “dry orgasm” or absence of ejaculation)Azoospermia is typically identified during a fertility evaluation with a semen analysis. Often, couples only discover it after months of trying to conceive without success, when testing reveals a zero sperm count.
Figure
In azoospermia, a man’s ejaculate contains no sperm (right), unlike a normal sample with millions of sperm (left). This condition can be due to blockages, testicular issues, hormonal problems, or other factors.
It’s natural to have questions: Does zero sperm mean the testes make none at all? Can it be a lab error? In many cases, confirmatory testing is done – the lab may centrifuge the semen to check for any tiny quantities of sperm, and a repeat semen analysis at a specialized lab is often recommended. Azoospermia can be classified into two broad types: obstructive azoospermia and non-obstructive azoospermia.
- Obstructive azoospermia means the testes are producing sperm, but a blockage or missing connection in the reproductive tract prevents sperm from appearing in the ejaculate. Men with obstructive causes have normal sperm production; the issue lies in the “plumbing.” Common examples include prior vasectomy, congenital absence of the vas deferens, or scarring of the ducts from infection or surgery. In these cases, sperm may be present inside the testicles or epididymis but can’t get out.
- Non-obstructive azoospermia means there is a problem with sperm production itself (a “factory” problem in the testes). This is also called testicular failure or secretory azoospermia. It can result from genetic conditions, damage to the testes, hormonal deficiencies, or other factors that impair the sperm-making process.
Distinguishing between these types is important because it guides treatment options. Doctors use clues from medical history, physical exam, and blood tests to figure out the likely cause. For example, a physical exam might find that the vas deferens (the tube carrying sperm) is absent or that the epididymis is swollen, pointing to an obstructive cause. Blood hormone levels, especially FSH (follicle-stimulating hormone), are also telling – a very high FSH suggests the testes are not producing sperm well (non-obstructive), whereas a normal FSH with low volume ejaculate might suggest an obstruction or absence of the seminal vesicles. In some cases, a genetic work-up is done, since certain genetic abnormalities can cause azoospermia (more on that below). Modern practice usually avoids diagnostic testicular biopsy unless absolutely needed, because often the cause can be deduced non-invasively.
Key point: A diagnosis of azoospermia should ideally be handled by a specialist (such as a urologist or reproductive endocrinologist) who can fully evaluate the male partner. Sometimes, azoospermia can be a sign of an underlying health issue (for instance, certain genetic syndromes or even an association with testicular cancer in rare cases), so it’s important the man’s overall health is assessed. But importantly, the specialist will help the couple understand their options for achieving pregnancy.
Why Might There Be No Sperm? – Causes of Azoospermia
There are many potential causes of azoospermia, and identifying the cause (when possible) can help determine the best path forward. Here are some common reasons a man may have no sperm in his ejaculate:
- Prior Medical Treatments: Chemotherapy or radiation therapy for cancer can severely affect sperm production. The testes are very sensitive to these treatments; as a result, some survivors of childhood or adult cancers have azoospermia due to treatment-induced testicular damage. (This is why oncology teams often recommend sperm banking before chemo/radiation when possible.) Similarly, surgical removal of both testes (e.g. for bilateral testicular cancer) obviously causes azoospermia. Some surgeries not involving the testes can also lead to azoospermia – for example, a retroperitoneal lymph node dissection (RPLND) for testicular cancer or surgeries on the bladder/prostate can damage nerves involved in ejaculation, leading to aspermia or retrograde ejaculation (where semen goes backwards into the bladder)Prior vasectomy is a very common surgical cause of obstructive azoospermia – it intentionally blocks sperm passage. Men who have had a vasectomy and later want children have the option of a surgical vasectomy reversal or sperm retrieval with IVF (discussed later).
- Genetic or Congenital Conditions: Genetics play a significant role in some cases of azoospermia. One well-known example is Klinefelter syndrome (47, XXY), in which men have an extra X chromosome; this often leads to very low or no sperm production. Another example is Y-chromosome microdeletions – tiny missing gene regions on the Y chromosome that are critical for sperm production (often termed AZF regions). If those genes are deleted, sperm may not be produced (tests can identify some of these deletions)There are also congenital issues like cryptorchidism (undescended testes) in childhood that, if uncorrected for years, can impair sperm development. Congenital bilateral absence of the vas deferens (CBAVD) is a condition typically associated with certain mutations in the cystic fibrosis gene; these men have normal sperm in testes but were born without the ducts (vas deferens) that carry sperm, resulting in obstructive azoospermia. (Many don’t realize they have this until infertility testing.)
- Hormonal Disorders: The process of sperm production is driven by hormones from the brain (pituitary gland). Low signals from the brain – for instance, due to pituitary gland tumors or genetic conditions like Kallmann syndrome – can cause a form of azoospermia where the testes are actually fine but not receiving the “start producing” signal. This is called pre-testicular azoospermia, and in some cases it can be treated with medications (like gonadotropin hormone injections to stimulate sperm production). On the flip side, external hormones can also cause issues: for example, men who take testosterone supplements or anabolic steroids can shut down their own sperm production (because the external testosterone suppresses the pituitary signals). This is usually reversible if caught in time and the hormone use is stopped, but prolonged steroid use can sometimes cause lasting problems.
- Ejaculatory or Sexual Dysfunction: Some men produce sperm but have difficulty ejaculating normally. Retrograde ejaculation is one instance – conditions like diabetes, spinal cord injuries, or prior surgeries (like prostate surgery) can cause semen to go into the bladder instead of out through the urethraIn such cases, a man’s semen analysis might show no sperm simply because the sperm went the wrong way. Often, doctors can detect this by checking the man’s urine after orgasm for the presence of sperm. Anejaculation(inability to ejaculate at all) can happen due to spinal cord injury or severe nerve damage. There are specialized techniques (vibratory or electrical stimulation) that can sometimes retrieve sperm in those cases. It’s worth noting that obstructive azoospermia (blockages) can be considered here too – for instance, a blockage in the ejaculatory ducts (where semen enters the urethra) due to cysts or scarring could present as no sperm in ejaculate. Some of these obstructive causes are treatable with surgery (e.g., a procedure called TURED can open blocked ejaculatory ducts).
- Idiopathic (Unknown) Causes: Despite thorough evaluation, many cases of non-obstructive azoospermia are idiopathic, meaning no specific cause is identified. Doctors suspect things like subtle genetic factors or developmental issues may be at play. As one expert source notes, “in most cases, though, azoospermia is likely due to factors we don’t fully understand, such as genetic conditions, poor testicular development as a fetus/child, or environmental toxins”. It’s important for couples to understand that not finding a cause is common and not their fault. The focus then shifts to what options exist given the situation.
Summary of Causes: Azoospermia can result from a range of issues – blockages (like vasectomy or absent vas deferens), testicular failure (genetic syndromes, damage from chemo, etc.), hormonal problems, or ejaculation dysfunction. Sometimes multiple factors overlap. Each couple’s case is unique, so working closely with a fertility specialist (often a reproductive urologist for the man) will clarify which category you fall into and what that means for treatment.
What to Do After a Zero Sperm Diagnosis – Medical Evaluation and Possible Treatments
When a semen analysis shows zero sperm, the next step is a comprehensive evaluation by a specialist. This usually involves: a detailed medical history, physical examination of the male partner, hormone blood tests, genetic tests if indicated, and sometimes imaging (like scrotal ultrasound) or other specialized tests. The primary goals are to identify any treatable cause and to determine if there might be any sperm recoverable through interventions.
Here are typical steps and considerations after an azoospermia diagnosis:
- Repeat Semen Analysis: First, the doctor may confirm the result with another semen test (often at a fertility-specialized lab). There can be variability between tests, and occasionally a few sperm might be found on a repeat exam (which could open up different options, like IVF with ICSI if even a small number of sperm are present). Ensuring the sample was produced correctly (with proper abstinence period, etc.) is also important. If even a rare sperm is seen on high-powered microscopic exam of a spun-down sample, the condition might be oligozoospermia (extremely low count) rather than absolute azoospermia – which can change the approach.
- Hormone Testing: Blood levels of hormones like FSH, LH, and Testosterone are checked. In non-obstructivecases where the testes aren’t making sperm, FSH is often elevated (as the pituitary is trying to stimulate the testes)A high FSH and small testicular size typically indicate testicular failure (non-obstructive azoospermia). Conversely, normal or low FSH with normal-sized testes might point toward an obstructive issue or hormonal suppression cause. If low gonadotropins (FSH/LH) are found, the doctor will look for causes in the brain/pituitary (and sometimes these can be treated with medication or surgery if, say, a pituitary tumor is found).
- Genetic Tests: Your doctor might recommend genetic screening. The standard tests often include a karyotype (to check for chromosomal abnormalities like Klinefelter syndrome) and specific tests for Y-chromosome microdeletions. If obstructive azoospermia with absence of the vas deferens is noted, genetic testing for CFTR gene mutations (cystic fibrosis gene) may be done because many men with CBAVD have subtle forms of cystic fibrosis mutations. Identifying a genetic cause is important not only for understanding prognosis (for example, some Y-chromosome deletions mean sperm retrieval is very unlikely) but also for family planning – some genetic causes could be passed on to children if you do find/use your sperm, so genetic counseling is advisable.
- Imaging and Physical Exam: A careful exam can sometimes find clues (like absence of vas deferens, as mentioned, or signs of hormonal problems such as small testes). Scrotal ultrasound might detect issues like varicocele (enlarged veins in the scrotum) – though varicoceles are a more common cause of low count rather than zero, they can contribute to testicular dysfunction. In obstructive cases, ultrasound might show dilation of structures like the epididymis. If a blockage at the level of the ejaculatory ducts is suspected, a transrectal ultrasound could be ordered. Each finding helps refine the diagnosis.
- Sperm Retrieval Attempts: Depending on the suspected cause, a doctor may suggest a procedure to try to retrieve sperm directly from the male reproductive tract. This is typically done by a specialized urologist. Techniques include:
- TESE (Testicular Sperm Extraction) – taking a small tissue biopsy from the testis to see if sperm are present inside.
- Micro-TESE (Microdissection Testicular Sperm Extraction) – an advanced version under an operating microscope, where the surgeon searches for tiny pockets of sperm production in the testesMicro-TESE has the highest yield for men with non-obstructive azoospermia and is often recommended in those casesIt can sometimes find sperm in ~50% or more of men who have no sperm in their semen, especially if some focal areas of sperm production exist. This sperm, if found, can be used to fertilize eggs via IVF with ICSI (intracytoplasmic sperm injection).
- Epididymal Aspiration (MESA/PESA) – extracting sperm from the epididymis (the duct behind the testes) via a fine needle or minor surgery, usually for obstructive cases like vasectomy or blocked vas deferens.
- Testicular Aspiration (TESA) – using a needle to aspirate tissue from the testes (sometimes done in obstructive cases or as a simpler initial attempt).
If an obstructive cause like a prior vasectomy is the issue, another option is a surgical reconstruction(vasectomy reversal or other microsurgery to bypass the blockage). Reversals can restore sperm to the ejaculate in many cases of vasectomy, which might allow natural conception or simpler intrauterine insemination (IUI) to be used rather than IVF. Your doctor will discuss the likelihood of success for these options based on your specific case. For example, in men who had a vasectomy many years ago, success of reversal may be lower and some couples opt directly for sperm retrieval plus IVF. In men with non-obstructive azoospermia, if hormonal therapy has any chance of boosting sperm production (like using medications for a few months), that might be tried prior to a surgical retrieval attempt – though evidence for medical treatments is limited in true testicular failure.
- Treat What’s Treatable: In a few fortunate cases, there are reversible causes. For instance, if a man is found to have a hormone issue like hyperprolactinemia (high prolactin) or thyroid imbalance, treating that might restore sperm production. If he’s on testosterone or anabolic steroids, stopping them (under medical supervision) and possibly using medications to kickstart the pituitary can sometimes lead to sperm returning in the ejaculate after several months. If a severe varicocele is present and other causes are unclear, surgery to repair the varicocele could be considered – although evidence is not definitive that this alone will cure azoospermia, some improvements have been noted in select casesIn obstructive cases such as an ejaculatory duct cyst, a minor surgery (TURED) can remove the blockage and allow sperm to flow again. Essentially, the medical team will address any fixable issues first.
After this process, you will reach a point where the doctor can give you a prognosis: either sperm has been found (or is likely findable with a procedure), or it appears that no usable sperm can be obtained from the male partner. If some sperm is retrieved (say via micro-TESE), couples can often use those sperm with IVF/ICSI to attempt pregnancy using the female partner’s eggs (if she is medically able) – this way the child is biologically related to both partners. However, not all retrieval attempts are successful. Especially in cases of severe non-obstructive azoospermia, despite best efforts, no sperm may be found in the testes. Or sometimes the male partner’s situation (e.g. genetic issues) makes even attempting retrieval inadvisable. At this juncture, the conversation often shifts to third-party reproduction options: namely, the use of donor sperm (or other donor gametes, or surrogacy depending on circumstances) to have a child.
It is completely understandable that many couples hold on to the hope that the male partner’s sperm can be used – and indeed, pursuing an expert evaluation is important to leave no stone unturned. But specialists also emphasize that even when no sperm can be obtained, it’s not “the end of the road” for parenthood. There are alternative paths that lead to a healthy baby and a happy family. As Johns Hopkins urology experts put it, “countless couples across the world have formed families with unsurpassed happiness and love by becoming parents by using donor sperm or by adopting an infant or child.” These are “completely acceptable paths for couples to choose”. In the next sections, we will explore the option of using donor sperm (either from a sperm bank or a known donor), as well as scenarios where donor eggs or a gestational surrogate might be needed, and important considerations around each.
Using Donor Sperm – How It Works and What to Consider

If the male partner’s sperm is not available or not viable for achieving a pregnancy, using donor sperm is a common and successful option. Donor sperm has been used for decades to help couples with male-factor infertility, single women, and LGBT couples have children. In fact, sperm donation for use in intrauterine insemination (IUI) or IVF has increased over the past 20 years, giving hope to many who otherwise could not conceive. The basic idea is that sperm from another man (the donor) is used to fertilize the female partner’s egg, resulting in a child who is genetically related to the mother (who provides the egg) but not to the father. This can be done through a relatively simple procedure like IUI (intrauterine insemination) or through IVF (especially if using IVF for other reasons like maternal age or if combining with donor eggs).
Here are key points and steps when considering donor sperm:
- Anonymous (Non-Directed) vs. Directed (Known) Donors: You can obtain donor sperm either from a sperm bank (where donors are typically anonymous or “non-directed,” meaning not personally known to you) or from a known individual (someone you and your partner recruit to donate – often called a directed donor). Both routes are viable, but there are differences. Sperm banks recruit and thoroughly screen donors; you usually select a donor profile (which may include characteristics like physical traits, education, hobbies, etc., and sometimes childhood photos or extensive biographies). Historically, these donations were anonymous, but many banks now offer Open ID donors – meaning the child can obtain the donor’s identity when they turn 18. On the other hand, a known donor could be a friend or even a family member of the intended father (some couples ask a brother or cousin of the male partner to donate, to retain a genetic link to the family). Using a family member as a donor is ethically acceptable with proper counseling and is sometimes chosen so that the child shares genes with the father’s family (for example, a brother’s sperm means the baby is the father’s genetic niece/nephew). This can help the infertile man feel a bit more “genetically connected” to the child. However, intra-familial donations raise special considerations like complex family dynamics and the need to guard against any pressure or coercion on the relative to donate. Thorough counseling and separate legal advice for all parties is a must in that case.
- Screening and Safety: Whether the donor is known or from a bank, medical screening is critical. Regulations (in the U.S., the FDA has specific rules) require that sperm donors undergo infectious disease testing, medical questionnaires, and in the case of anonymous donors, a quarantine of samples for six months with re-testing before release. Donor sperm from a licensed bank will have been tested for diseases like HIV, hepatitis, syphilis, gonorrhea/chlamydia, etc., and also usually for common genetic carrier conditions. ASRM guidelines outline extensive screening: a good donor should be healthy, with no significant hereditary diseases, and have excellent sperm parameters. Psychological evaluation of the donor is also recommended. If you use a directed (known) donor, the FDA still mandates infectious disease testing within 7 days of donation. Interestingly, if a known donor has a finding that would make them “ineligible” by anonymous donor standards (say they carry a genetic trait or have a positive test for CMV), the FDA does allow their sperm to be used for that specific recipient if both parties are aware of the risks and consent. For example, a brother who is a carrier of a recessive genetic disease could still donate to his sibling if everyone understands the implications. Clinics typically still follow rigorous screening and often quarantine even known donor sperm for 30–35 days with re-testing to increase safety. One thing to note: using fresh (unfrozen) donor sperm is generally not recommended unless the donor is the spouse/intimate partner. Fresh donations from third parties carry a risk of transmitting infections before tests can detect them, so almost all programs use frozen, quarantined donor sperm to be safe.
- Process of Donor Insemination or IVF: If the female partner has no fertility problems and is relatively young, many couples choose to start with IUI using donor sperm. This involves tracking the woman’s ovulation (or stimulating ovulation with medicine) and then inserting the donor’s sperm directly into her uterus at the right time. It’s a straightforward office procedure. Success rates per IUI cycle with donor sperm can vary (often around 15-20% per try, depending on the woman’s age and fertility health). It may take a few cycles. If there are any female fertility issues (like blocked fallopian tubes or advanced age), or if multiple attempts at IUI haven’t succeeded, IVF with donor sperm might be recommended. With IVF, the woman’s eggs are retrieved and fertilized with the donor sperm in the lab (via ICSI if sperm count/motility is an issue, though donor sperm usually has high counts). IVF has higher per-cycle success rates and also allows for additional options like genetic testing of embryos if desired. In either IUI or IVF, you will typically purchase vials of frozen sperm from the bank, which are shipped to your clinic. Donor sperm is usually sold in units (vials), and your doctor will advise how many vials to have on hand per cycle (often one per IUI attempt, more for IVF just in case). If using a known donor, the sperm can be collected at a clinic, frozen and quarantined, then used similarly.
- Emotional Journey and Partner Feelings: Deciding to use donor sperm is a significant emotional step for many couples. It is normal for both partners to experience a mix of emotions – grief over the loss of the genetic connection for the male partner, concerns about family acceptance, or worries about whether the non-genetic father will feel like “the real dad.” Men may experience feelings of inadequacy, guilt, or fear that the child won’t bond with them. Women may have complex feelings too – empathy for their partner’s pain, or even worry that using another man’s sperm feels “wrong” or like a breach of trust. These reactions are common and valid. It often helps to acknowledge and grieve the loss of a purely biological child together, and many couples find benefit in talking with a therapist specialized in fertility or donor conception. In fact, fertility clinics frequently require or recommend counseling before third-party reproduction, to help intended parents process feelings and plan for the future. One key message from mental health professionals is that having a child via donor sperm is just a different way of building a family – and it can be just as joyful and fulfilling. The non-genetic father is the real father in every social and emotional sense that matters. Over time, most couples report that once their child is born, the genetic issue recedes in importance – the day-to-day reality of parenting takes over, and love grows naturally. But getting to that point may involve working through some tough feelings, and that’s okay. It’s important for couples to communicate openly, support each other, and perhaps connect with others who have gone through it (there are support groups for donor conception).
- Talking to Others and to Future Children: A big question is often, “Do we tell people (friends/family) that we used a donor? And do we tell the child someday?” This is a personal decision, but there is a strong trend in recent years toward openness, at least with the child. Experts generally encourage being honest with children about their donor conception from an early age in an age-appropriate way. The reasoning is that secrecy can unintentionally introduce shame or stigma, whereas treating it as a normal part of the child’s story helps them develop a secure identity. Moreover, with modern DNA testing (think 23andMe, Ancestry.com, etc.), secrets are very hard to keep – many donor-conceived individuals end up discovering their origins through DNA matches even if their parents never told them. Finding out late (or by surprise) can lead to feelings of betrayal in some cases. In contrast, studies show that kids who grow up always knowing they were donor-conceived (because their parents told them from young age) generally take it in stride and have no issues embracing both their non-genetic parent as “real mom/dad” and understanding the special way they came into the world. Many parents choose to frame it positively: e.g., “We wanted you so much we needed a special helper to get you here, and we are so glad you’re you.” That said, the decision of who else to tell (outside the immediate family) is up to you. Some couples worry about nosy relatives or social stigma. You are not obligated to share details with everyone; however, keeping an absolute secret within the immediate family can be hard long-term. Some men initially feel they only can accept the plan if nobody ever knows – but consider that this might put a burden on the family (and the child) to keep a lifelong secret. Over time, comfort levels often increase, and many people end up telling close family or friends for support. There are resources (books, counselors) to help navigate these conversations.
- Success Rates and Building Your Family: Using donor sperm is a highly successful approach. If the female partner is healthy and of a favorable age, chances are good you can conceive a child this way. Many couples who go this route have happy outcomes. It might not happen on the first try – like any fertility treatment, there can be ups and downs. But keep faith. One reassuring fact: there have been thousands upon thousands of babies born via donor sperm. You are truly not alone, and this method is an established part of reproductive medicine. As an example, a U.S. survey in 1995 estimated about 170,000 women had used donor sperm in their lifetime (and that was decades ago) – the number is likely much higher now. Fertility clinics and sperm banks have a lot of experience guiding couples through this.
- Cost and Logistics: Donor sperm is one of the more affordable third-party options, especially if using IUI. Each vial of donor sperm may cost a few hundred to a thousand dollars, depending on the bank and the donor’s characteristics (some banks charge more for donors with certain characteristics or proven pregnancies). Insemination procedures and fertility monitoring add to the cost. If IVF is done, costs are higher (IVF cycles can be several thousands of dollars). Some insurance plans cover fertility treatments except donor components; others might cover inseminations. It’s worth checking your coverage. Additionally, if you anticipate wanting more than one child using the same donor (for genetic siblings), you may consider purchasing extra vials and storing them, as donor supply can run out once a donor retires or reaches family limits. Coordinate with your clinic’s recommendations.
In summary, choosing donor sperm is a big decision, but it is a lifeline for many couples after the blow of an azoospermia diagnosis. It transforms the situation from “no chance” to “a very real chance of having a baby.” Both anonymous sperm bank donors and known donors are options, each with pros/cons. Careful screening makes the process safe. The emotional journey may have complexities – grief, acceptance, and eventually joy – so utilize counseling and support resources (like RESOLVE support groups, or online communities for donor conception). And remember that using a donor is simply one way to build a family; love, parenting, and lifetime commitment are what truly make a father or mother, not just genes.
When Additional Help Is Needed – Donor Eggs, Surrogacy, and More
In some cases, the challenge isn’t only the male partner’s lack of sperm. What if the female partner also has fertility issues? For example, the woman might have no viable eggs due to premature ovarian failure or prior cancer treatment, or she might be unable to carry a pregnancy because she doesn’t have a uterus (due to hysterectomy or a congenital condition) or has a medical condition that makes pregnancy unsafe. These situations can compound the difficulty, but there are still solutions available. They may involve multiple third-party contributors – such as both donor sperm anddonor eggs, or donor embryo, plus possibly a gestational surrogate to carry the pregnancy. This is often referred to as third-party reproduction or collaborative reproduction, since people beyond the couple are helping in the process.
Let’s break down scenarios and options:
- If the Male has No Sperm and the Female Partner Needs Donor Eggs: This scenario could occur if, say, the male partner has azoospermia and the female partner has diminished or absent ovarian function (due to age, premature menopause, chemotherapy, genetic issues like Turner syndrome, etc.). In this case, the couple would need both a sperm source and an egg source. One approach is to use donor sperm + the female partner’s own eggs (if she still has some). But if she truly has no viable eggs, the next option is to use a donor egg (oocyte) as well. Donor egg IVF involves a young woman (the egg donor) undergoing ovarian stimulation and egg retrieval, and those eggs are fertilized (in vitro) with sperm – which in our case would be donor sperm since the male has none. The resulting embryos can then be transferred into the female partner’s uterus, and she can carry the pregnancy if her uterus is intact and healthy. The child would be genetically related to neither intended parent in this case (biologically, the child would have the egg donor’s genes and the sperm donor’s genes), but the female intended parent would be the one to nurture the pregnancy and give birth, and both intended parents would be the child’s parents in every social/legal sense. Another option, if both egg and sperm are donated, is sometimes called embryo donation/adoption – where the couple receives a donated embryo (often leftover from another couple’s IVF) and the female carries it. This is conceptually similar to using both donors, except the embryo is already created. Embryo donation can be a cost-effective and altruistic route (since many embryos are donated by couples who want to help others). The ASRM and fertility societies have guidelines for embryo donation to ensure proper screening and consent. The process legally can resemble adoption in some ways, hence it’s sometimes called embryo adoption (though not a legal adoption of a born child, but rather a transfer of ownership of embryos with consent of donors and recipients).
- If the Female Partner Cannot Carry a Pregnancy (No Uterus or Health Contraindication): In situations where the woman has eggs (or can use donor eggs) but cannot carry (for example, she had a hysterectomy due to cancer or a severe uterine condition, or she has a serious heart condition that makes pregnancy dangerous, or perhaps a same-sex male couple or single man wanting to have a child), the option is to use a gestational carrier, commonly known as a surrogate. A gestational carrier (GC) is a woman who carries a pregnancy for the intended parent(s) but has no genetic relation to the baby – the embryo is created from either the intended mother’s egg or a donor egg and the intended father’s sperm or donor sperm, and then transferred into the GC’s uterus. The GC is essentially the birth mother but not the genetic mother. (This is different from the older concept of “traditional surrogacy,” where the surrogate’s own egg is used; traditional surrogacy is rarely done now because of legal and emotional complexities. Almost all surrogacy today is gestational surrogacy.) Using a gestational carrier is a well-established practice for cases where carrying a pregnancy is not possible for the intended mother. For example, women with Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome, who are born without a functional uterus, often use gestational surrogacy to have genetically related children using their own eggs. Another example is a woman who had her uterus removed but still has ovaries – she can do an egg retrieval, create embryos with her partner’s sperm, and have those embryos carried by a surrogate.
- Gestational Surrogacy – Key Facts: If you are considering a surrogate, it’s important to know the general process and safeguards:
- Surrogates (carriers) are typically healthy women between 21 and 45 years old who have already had at least one uncomplicated pregnancy of their own. Having prior successful pregnancies is usually a requirement because it demonstrates fertility and also ensures the surrogate understands the physical and emotional aspects of pregnancy. ASRM guidelines suggest certain limits (for example, no more than 5 previous deliveries, and if any C-sections, not too many).
- The intended parents undergo IVF to create embryos (using either their own gametes or donors as needed). Those embryos are then transferred into the surrogate’s uterus. The surrogate carries the pregnancy to term and delivers the baby, which is then given to the intended parents.
- Surrogacy involves intensive screening: The carrier will have a full medical work-up to make sure her uterus and health are suitable for pregnancy. She will also undergo psychological evaluation and counseling. Any spouse/partner of the surrogate may be included in counseling too, since the pregnancy can affect her family. The intended parents also typically have counseling, to prepare for the unique relationship with the surrogate and to discuss issues like how they will handle communication during and after pregnancy.
- Legal contracts are absolutely critical in surrogacy. Each party (the intended parents and the surrogate) must have independent legal counsel experienced in reproductive law. The contract will cover everything from the surrogate’s medical care and responsibilities, to agreements on pregnancy management (for instance, how many embryos will be transferred, views on selective reduction or pregnancy termination if complications arise), to financial compensation, and plans for after birth (like pumping breast milk or not, contact arrangements, etc.). It also spells out that the surrogate intends to relinquish the child to the intended parents and their intent to assume parentage.
- Compensation: In many places (including most of the U.S.), surrogates are compensated for the significant time, discomfort, and risk they undertake (in addition to all medical bills being covered by the intended parents). Surrogacy is ethically considered acceptable to compensate, as long as it’s not exploitive. The amount can vary but generally covers pregnancy-related expenses plus an agreed fee. Some jurisdictions, however, only allow altruistic surrogacy (no payment beyond expenses).
- Legal Parenthood: The ultimate goal is that the intended parent(s) are recognized as the legal parents of the baby. Laws on this vary by state and country. In many U.S. states, you can obtain a pre-birth court order declaring the intended parents as the legal parents (often the birth certificate is then issued directly with their names). In other cases, a post-birth process or adoption may be needed. It is vital to work within the law – as ASRM’s Ethics Committee emphasizes, “The intended parents should be the legal parent(s) of any child born to a GC. Any arrangement in a jurisdiction that does not ensure that should be considered with caution and only with advice of independent legal counsel.”. In other words, if a state’s laws wouldn’t automatically make you the parent (say the law might treat the surrogate as the mother by default), you must plan legal steps to secure your parental rights and perhaps reconsider doing it in that state.
- Surrogacy by the numbers: It’s becoming more common. Between 1999 and 2013, the percentage of IVF cycles using gestational carriers in the U.S. rose from 1% to 2.5%, and by 2019 it was around 5.4% of all IVF cycles. This includes use by not just infertile couples, but also same-sex couples and others. Studies have shown that IVF success rates with surrogates can be as good as or better than average (likely because the surrogates are screened for optimal health). Surrogacy has enabled many to have children where it was otherwise impossible – for instance, after uterine cancer, or for male gay couples where one provides sperm and either an egg donor is used or one partner’s sister donates an egg so each father has a genetic link, etc.
Infographic from ASRM’s ReproductiveFacts: Gestational Carrier vs. Surrogate. A gestational carrier (GC)carries a pregnancy for intended parent(s) but is not genetically related to the baby (the embryo is created from the IPs’ or donors’ gametes via IVF). In contrast, a “traditional” surrogate provides her own egg and carries the baby, making her the genetic mother – a practice now rare due to legal complexity. Modern surrogacy almost always uses a GC approach to avoid the surrogate having a genetic tie to the child.
- Combining Solutions: There are cases where a couple might need a combination of donor sperm, donor egg, and a gestational carrier. For example, imagine a couple where the man has no sperm and the woman cannot produce eggs and also cannot carry (perhaps due to a medical condition). Though this is a lot of hurdles, even here a path exists: the couple could have an embryo created from a donor egg fertilized by donor sperm, and then have that embryo gestated by either the female partner (if her uterus works but she had no eggs) or a surrogate (if she also has no uterus or it’s unsafe). In that scenario, the child is not genetically related to either parent – genetically, the child comes from two donors – but the intended parents are the ones who will raise the child and be on the birth certificate (especially if a proper legal process is followed). Some couples consider this akin to adoption, except they are able to experience the pregnancy (in the case where the intended mother can carry a donor embryo) or at least have a newborn child from birth via surrogacy. Others might decide that if neither of them can contribute genetically, they prefer to pursue adoption of a living child instead of creating an embryo from donors. Adoption is certainly an alternative path to parenthood outside of the medical sphere, and it can be a beautiful option for many. It has its own process, costs, and considerations separate from the fertility clinic route. There is no right or wrong choice – it’s about what resonates for you as a couple.
- Support and Decision-Making: Facing the need for multiple third-party interventions can be emotionally daunting. It’s important to engage in thorough discussions with your fertility specialist and possibly a counselor. Ethical and psychological counselling is strongly advised whenever donor gametes or surrogates are involved. This helps ensure everyone is on the same page about the implications (for example, discussing how a child resulting from donor egg and donor sperm will have no genetic link to the parents, and how/when that might be explained to the child). It’s also crucial to consider the long-term: With more than one donor involved, a child may someday have interest in their genetic origins. Many donors nowadays (egg or sperm) are willing to be contacted when the child is grown (open-ID donors). There are also registries to connect donor-conceived siblings (e.g., the Donor Sibling Registry). Being emotionally prepared for these future possibilities (while still maintaining that you are the parents in the child’s life) is part of the journey.
- Success Rates with Donor Eggs/Embryos: Using donor eggs tends to have high success rates because donors are usually young and fertile. IVF with donor eggs for a woman who couldn’t conceive with her own eggs often dramatically increases the chance of pregnancy. Surrogacy success will depend on the quality of the embryo and the surrogate’s uterine receptivity, but surrogates are chosen for their proven fertility, so success is generally high as well. Many couples who undergo these processes do achieve a baby, even if it’s not the way they originally envisioned.
Takeaway: Even when fertility challenges affect both partners, modern medicine provides avenues to parenthood. Donor eggs, donor sperm, and gestational carriers can be used in various combinations to overcome almost any biological barrier to having a child. While the idea of involving third (or fourth) parties in creating your family can initially be uncomfortable, many couples ultimately find great fulfillment and joy in these solutions. It’s essential to seek care at a reputable fertility center with experience in third-party reproduction, undergo proper counseling, and surround yourself with support. At the end of the day, the goal is achieving a healthy child and for you to become parents – and there are multiple paths to reach that goal, even if both your egg and sperm are not usable.
Legal and Ethical Considerations (Donors and Surrogacy)
Whenever third-party reproduction is involved – be it using a sperm donor, egg donor, or a surrogate – there are important legal implications to address. Laws vary by jurisdiction, and the rights and responsibilities of each party must be clearly defined to protect everyone involved (especially the intended parents and the child). This section highlights key legal considerations and why consulting an experienced reproductive law attorney is imperative.
Using Donor Sperm (or Eggs):
In the United States, there are generally well-established legal frameworks that consider a sperm donor (who is not the intimate partner of the woman) not to be a legal father, provided the donation was done through a physician or sperm bank. Most states have statutes (often based on the Uniform Parentage Act) which say that if a man donates sperm to a woman (other than his wife) via a licensed physician for use in artificial insemination, he has no parental rights or obligations to any resulting child. This is what allows anonymous donor sperm to be used without the donor later claiming the child, and also prevents donors from being liable for child support. However, if you do not follow the proper procedure (for example, a private arrangement at home without a doctor’s involvement), you could run into legal trouble. A famous case occurred in Kansas: a man privately donated sperm to a lesbian couple for home insemination, and years later the state pursued him for child support because the insemination wasn’t done through a physician, so the law did not recognize him as a protected donor. Even though he and the couple had signed a contract waiving his parental rights, the court ruled that the state law’s requirements trumped that agreement, and since no doctor was involved, he was on the hook as a legal father. (Eventually, after much legal battle, a judge later clarified he wasn’t the father, but only after significant distress and cost.) The lesson is clear: always use a proper medical setting for donor insemination and have legal contracts in place. If you are using a known donor, both the donor and the intended parents should sign a donor agreement before any procedures. This agreement usually states the donor relinquishes any parental rights, the intended father (if any) will be the legal father, and outlines confidentiality or future contact intentions. While a contract cannot override certain state laws (like in the Kansas case), it is still an important piece of evidence of everyone’s intent and is often required by clinics.
For egg donors, similar principles apply: an egg donor typically signs away parental rights in the donation contract, and by law the birth mother (whether the intended mother or a surrogate) is the legal mother of the child. Embryo donation also requires contracts where the donor couple relinquishes any claim to resulting children.
It’s worth noting, anonymity in donation is not ironclad in the modern era of DNA testing. Donors who expected to remain anonymous could be identified later by DNA connections. This doesn’t affect legal parentage (the donor is still not the legal parent), but it’s something to be aware of when considering future privacy and family dynamics.
Surrogacy – Legal Points:

Gestational surrogacy is legal in many places, but the specific laws can differ dramatically by state (and country). Some U.S. states have statutes that explicitly permit surrogacy and outline how to establish the intended parents’ rights. For example, California and Connecticut are known for being surrogacy-friendly, granting parentage orders easily. Other states are more restrictive or have unclear laws; a few (like Michigan) actually prohibit paid surrogacy agreements and might even impose penalties. Most states fall somewhere in between – allowing it under certain conditions. That’s why one of the first steps if you pursue surrogacy is to engage a lawyer and ensure you plan the process in a jurisdiction where your parental rights can be secured.
Key legal aspects for surrogacy include:
- Surrogacy Agreement: This detailed contract, drawn up before pregnancy (and usually before embryo transfer), sets forth everyone’s obligations and expectations. It covers the surrogate’s compensation, medical expenses, insurance, agreement to follow certain medical guidance (for example, taking prenatal vitamins, abstaining from alcohol/drugs, etc.), what happens in case of pregnancy complications or multiple pregnancy, and clauses on sensitive issues (such as how decisions about pregnancy reduction or termination would be handled if medically needed – often the intended parents have decision-making power in consultation with doctors, but these things must be explicitly agreed on to avoid disputes). The contract also typically requires that the surrogate will hand over the baby to the intended parents at birth and cooperate in any legal proceedings to establish their parentage. It will also clarify things like the surrogate’s ability to make healthcare decisions during pregnancy (day-to-day decisions are usually hers, but major decisions often involve the IPs) and plans for contact during the journey. Both parties have separate lawyers to ensure fairness.
- Parental Orders or Adoption: Depending on the state, lawyers will either file a pre-birth order (during the pregnancy) or a post-birth petition to declare the intended parents (IPs) as the only legal parents. If the IPs are married and at least one of them is a genetic parent (e.g., the father’s sperm was used), many states will issue a pre-birth order so that hospital will treat them as the parents from the first moment. If an egg donor was used and only the father is genetically related, sometimes the non-genetic intended mother might formally adopt the baby after birth (second-parent adoption) in certain states, but in surrogacy-friendly states a pre-birth order can often include a non-genetic mother as well by acknowledging the intent and the egg donor’s renouncement of rights. It’s crucial to follow the correct procedure as advised by the attorney. The goal is to avoid any scenario where the surrogate (or anyone else) is erroneously considered a parent on record. When done correctly, the surrogate should not have her name on the birth certificate at all, and she has no rights or obligations to the child.
- Surrogate’s Rights and Protection: Good surrogacy practices also ensure the surrogate has rights protected. She has the right to medical care and support, the right to independent legal counsel (paid for by the IPs, usually), and the right to make informed decisions about her own health. Ethically, the surrogate always maintains bodily autonomy – meaning she cannot be forced into medical procedures or treatments without consent, even if agreed in contract (courts generally won’t enforce anything that violates a person’s bodily autonomy). Thus, a relationship of trust and communication is important. Additionally, surrogates should have life insurance (often provided via the contract) and sometimes additional health/disability coverage in case of pregnancy complications.
- Ethical Considerations: Surrogacy has some debated ethical issues. Critics worry about exploitation – e.g., women feeling pressured or doing it purely for financial need. That’s why screening and fair compensation are important to ensure she’s doing it willingly and is financially stable enough that it’s not an act of desperation. Supporters point out that, with proper safeguards, surrogacy can be empowering and beneficial for all parties. Studies have found that many surrogates and intended parents report positive experiences and strong mutual respect. Nonetheless, it’s a field where ethical guidelines stress the importance of thorough counseling and ensuring everyone’s on the same page morally. For instance, all parties should discuss and agree on what will happen if a serious fetal abnormality is detected – would termination be an option or not? These value-laden topics must be addressed upfront to avoid conflict later.
- International Considerations: If you are reading this outside the U.S., be aware that some countries ban all forms of surrogacy (e.g., France, Germany) while others allow only altruistic surrogacy (e.g., Canada, UK – where paying only reasonable expenses is allowed, not a fee). Some countries (like Ukraine, Georgia, certain U.S. states, etc.) allow compensated surrogacy and have well-established frameworks. There are also countries where surrogacy was popular but legal changes occurred (for instance, India had a booming surrogacy industry but now heavily restricts it to citizens). International surrogacy can be legally complex in terms of citizenship and bringing the baby home, so it requires navigating both the birth country’s and your home country’s laws.
Legal Advice Is a Must: Given all the above, one cannot overstate the importance of getting proper legal advice when using donors or surrogates. Before you even begin (for example, before your known friend provides a sperm sample, or before you start an egg donor cycle, or sign up with a surrogacy agency), consult a lawyer who specializes in reproductive law in your jurisdiction. They will guide you on necessary contracts and steps to ensure that you are recognized as the legal parents and that donors/surrogates do not retain any unintended rights or liabilities. In the U.S., organizations like the American Academy of Reproductive Lawyers (AARTA) can help locate qualified attorneys.
A quick note on finance/legal: especially with surrogacy (and sometimes egg donation), escrow accounts are used to handle the payments to the surrogate or donor via a neutral third party, per the contract schedule. This is to protect both sides financially.
Finally, beyond the law, consider the ethical dimension for your family: If you use a donor, think about future curiosity the child may have, and consider keeping information that might help them (many parents keep the donor profile, donor ID, and any correspondence). If you use a surrogate, think about what relationship, if any, you’d like to have with her after birth (some remain in touch, even visiting; others have a more transactional but respectful relationship). There’s no single correct way, but being thoughtful and compassionate with all involved will serve you well.
Coping and Support – You Are Not Alone

Dealing with infertility and the realization that you may need outside help to have a child can be emotionally taxing. It’s normal to feel grief, anger, anxiety, or isolation. Both partners can experience a sense of loss – for the man, loss of genetic fatherhood; for the woman, possibly the loss of the “natural” path to pregnancy, or empathy pain for her partner. Couples might feel strain in their relationship as they process this. It’s crucial to know that support is available and that many couples have gone through this journey and come out stronger.
Emotional Stages: Many individuals go through stages similar to grieving – denial, bargaining, sadness, eventually towards acceptance. It’s okay if you need time to decide on donor conception or other options; don’t rush your emotions. Some men struggle particularly because male-factor infertility can challenge societal notions of masculinity, making them feel embarrassed or “less manly.” This can lead to withdrawal or reluctance to talk about it. Women might cope by seeking support, talking, researching, whereas men might initially shut down or attempt to cope silently. Recognize these different coping styles and try not to blame each other. Instead, encourage gentle communication. Sometimes writing feelings in a journal or letter can help express what’s hard to say out loud.
Professional Counseling: Seeing a therapist who specializes in infertility or a couples counselor can be enormously helpful. In fact, ASRM recommends psychoeducational counseling for anyone pursuing third-party reproduction. A therapist can provide a safe space for both of you to voice fears and hopes, and help you navigate disagreements (for example, one partner might be more ready for donor sperm than the other initially – therapy can help bridge that gap by addressing concerns). They can also guide you on how to eventually talk to your child about their conception story. Many fertility clinics have mental health professionals on staff or can refer you. Don’t think of it as something being “wrong” – think of it as adding an expert to your team to ensure you are emotionally healthy going into this new chapter.
Support Groups: Sometimes, talking to peers who “get it” is uniquely empowering. Consider joining an infertility support group. The organization RESOLVE: The National Infertility Association offers support groups across the U.S., including some specifically for men, or for those considering donor conception. Hearing from others who used a sperm donor or surrogate and now have a child can be incredibly comforting – living proof that this can work out and that their families are normal and happy. Online forums and communities also exist (though be mindful to use reputable ones, as some unmoderated forums can sometimes increase anxiety). There are also groups like the Donor Conception Network (originally UK-based) which have resources for parents and donor-conceived children, and the Donor Sibling Registry where you could connect with genetic half-siblings if using the same donor becomes a consideration. Engaging in these networks can reduce the feeling of isolation.
Talking to Family: Deciding how much to share with your extended family or friends is personal. Some couples choose to be very open about using donor sperm or surrogacy; others prefer to keep it private. There is no obligation to divulge your medical history or family-building method if you don’t want to. That said, having at least one or two confidants (a close friend or a sibling/parent you trust) can provide a pillar of support. If you expect support rather than judgment from certain people in your life, letting them in on your plan can relieve the “secret-keeping” stress and allow them to cheer you on. With surrogacy, it often becomes known to family/friends simply because the intended mother is not physically pregnant – having a prepared explanation like “We’re working with a gestational carrier who is helping us have our baby” can be helpful. You might be surprised – many people are more understanding and excited for you than you’d expect. Infertility is very common, and you may find empathy or even discover others who had similar experiences.
Self-Care: Throughout this process, remember to take care of your relationship and yourselves. Infertility can become an all-consuming project. Make time to do things unrelated to baby-making – whether it’s date nights, hobbies, exercise (which helps mood), or short getaways. Continue to nurture your intimacy in non-baby-focused ways so that sex isn’t only associated with fertility schedules (especially since with donor sperm, conception might occur via procedure rather than intercourse, which can affect a man’s sense of involvement – find other ways to maintain physical and emotional intimacy). Some couples find strength in their faith or spirituality during these times; others find meaning in volunteering or focusing on areas they can control.
Hope and Outlook: It bears repeating that having a child is still very much possible, even if the usual route is closed. The majority of couples who pursue donor gametes or surrogacy do succeed in having children. The technology and expertise available today are astounding – what was science fiction a generation ago is routine now. For example, there are cases of men with non-obstructive azoospermia who, thanks to micro-TESE, had a few sperm found and now have genetic children. And for those who cannot retrieve sperm, donor sperm has enabled parenthood for countless families. Surrogacy has allowed women without a uterus to have a baby and experience motherhood. Try to focus on the end goal: a healthy baby in your arms. The genetics and the process are just the means to that end. Once you’re holding your child, the love you feel does not depend on DNA.
In tough moments, it might help to recall why you’re going through all this – because you deeply desire to parent together. Keep the image of your future family in mind. And also know when to give yourselves a break from the process if needed; it’s okay to step back and recharge if treatments or decisions become too stressful.
Lastly, know that society’s understanding of these issues is improving. There’s less stigma than before around infertility and using IVF or donors. Advocacy groups and medical professionals have worked hard to spread the message that infertility is a medical condition – not a reflection of someone’s worth or identity. You deserve support and compassion, not stigma.
Support Resources (U.S. and International):
- RESOLVE: The National Infertility Association – provides support group listings, educational resources, and advocacy.
- American Society for Reproductive Medicine (ASRM) – has patient fact sheets, and an online community “inspire” forum in partnership with RESOLVE for those dealing with infertility and donor issues.
- Mental Health Professionals (MHPG directory via ASRM) – find a therapist who focuses on infertility.
- Donor Conception Network (DCN) – a network based in the UK with resources for donor-conceived families (useful readings and support even if you’re elsewhere).
- Donor Sibling Registry (DSR) – helps connect families with genetic links via the same donor and provides a space for donor-conceived persons (if open identity is desired down the road).
- Fertility Clinics’ Counseling Services – many clinics have on-staff counselors or can refer you locally.
- Books – There are memoirs and books by parents who used donor sperm or surrogacy which can provide insight and comfort. Titles like “Three Makes Baby” (a guide to donor-conceived family parenting) or “Flowers From Love: The Donor Sperm Journey” (anecdotal) might be worth exploring.
- Blogs –
- https://mensreproductivehealth.com/why-do-couples-use-a-gestational-carrier-or-surrogate/
- https://mensreproductivehealth.com/genetic-carrier-screening-and-donor-eligibility-in-ny-a-guide-for-clinics-and-patients/
- https://mensreproductivehealth.com/content/male-donor-eligibility-qualification/
- https://mensreproductivehealth.com/content/directed-donor/
Conclusion
Facing the reality that your partner has no sperm can be one of the most challenging hurdles on the road to parenthood. It’s a diagnosis that upends the expectation of conceiving naturally, and it’s normal to feel a sense of loss. Yet, as we’ve discussed, it is far from the end of the road. Modern fertility medicine offers an array of options – from using donor sperm, to incorporating donor eggs, to enlisting the help of a gestational carrier – that can make your dream of having a child come true, even if the traditional genetic route isn’t available.
What’s most important is that you and your partner approach these options united and informed. Take the time to learn about each path, speak to doctors and counselors, and reach a decision that you both are comfortable with. There is no “one-size-fits-all” right answer – some couples immediately feel okay with using a sperm donor, while others may need longer to warm up to the idea; some may draw the line at how many “third parties” they are willing to involve, whereas others are open to whatever it takes. Honor your own values and feelings, and proceed at the pace you need. Remember that choosing an alternative path does not make the child any less “yours.” Parenting is built on love, care, and commitment. As many who have gone before will attest, when you hold that baby – however they came into existence – you will know deep down that they are your child and none of the early struggles will change that bond.
One day, this chapter of infertility and tough choices will just be part of your family’s origin story – perhaps even one that you’ll share with pride about the lengths you went to for your child. As one resource beautifully put it: “We wanted to have you so badly that we went to great lengths to find help. We’re so glad you’re you, and we’re so glad you’re ours.”.
In the meantime, lean on available resources. Build a support system, whether personal or professional. Ensure the legal details are handled so you can move forward smoothly. By educating yourself (as you’re doing now), you are already taking empowering steps.
Your journey might have detoured into territory you never expected, but it can still lead to the destination you yearn for – a happy, healthy family. Many others have walked this path and now tuck their children in at night, grateful for the science and donors and surrogates that helped them become parents. With the right help and information, you can join their ranks. Keep hope alive, take care of each other, and look ahead to the new possibilities. The absence of sperm is a challenge, but it’s one that can be overcome with compassion, creativity, and support.
Above all, remember: You are not alone, and your dream of having a child is still very much within reach.
Subscribe to our weekly blog here:
References:
- Brannigan RE, et al. Updates to male infertility: AUA/ASRM guideline (2024). J Urol. Published online Aug 15, 2024. (Male factor involved in ~50% of infertile couples; evaluation and management guidance)
- Sharma M, Leslie SW. Azoospermia. StatPearls [Internet], Updated Nov 18, 2023. (15% of couples infertile; azoospermia in 1% of men and 10–15% of infertile men)
- Johns Hopkins Medicine. Azoospermia – Condition and Diseases. (Definition of azoospermia; causes including Klinefelter’s, chemo, vasectomy; reassurance about donor sperm/adoption paths)
- ASRM Practice Committee. Guidance on Gamete and Embryo Donation. Fertil Steril. 2024;122(4):799–813. (Use of donor gametes has increased; donor screening standards and directed vs non-directed donation)
- Feingold ML, updated by TSBC 2022. Heterosexual Couples Using Donor Insemination – The Sperm Bank of California. (Emotional aspects of using donor sperm; 15% of couples infertile; importance of communication and disclosure)
- UCSF Center for Reproductive Health. Donor Sperm for Male Infertility. (Overview of using donor sperm; support resources like Resolve, Donor Conception Network, DSR)
- Ethics Committee of ASRM. Using Family Members as Gamete Donors or Surrogates. Fertil Steril. 2024. (Intrafamilial sperm donation can preserve genetic ties; must ensure informed consent and avoid coercion)
- Ethics Committee of ASRM. Consideration of the Gestational Carrier: an Ethics Opinion. Fertil Steril. 2023. (Defines GC vs traditional surrogate; ethical use of surrogacy; need for separate legal counsel and that IPs be legal parents)
- ReproductiveFacts (ASRM) Patient Fact Sheet. Gestational Carrier (Surrogate). Revised 2023. (Indications for GC use – absence of uterus or medical contraindication; recommended criteria for surrogates – age 21–45, prior healthy pregnancy)
- Stange Law Firm article. Kansas Court Ruling: Sperm Donor Ordered to Pay Child Support. March 13, 2025. (Kansas case of donor liable for support due to no physician in insemination; importance of following state law for donor arrangements)
- World Health Organization. News release: 1 in 6 people globally affected by infertility. April 4, 2023. (Approximately 17.5% of the adult population experiences infertility, showing it’s a common global issue)
- Cleveland Clinic. Azoospermia (Zero Sperm Count) – Patient Education. (Explains obstructive vs non-obstructive azoospermia; mentions 1% of men have it; graphic depiction of condition)
- Chang J, et al. Estimates of Donated Sperm Use in the United States. Fertil Steril. (Data from 1995 estimated ~170,000 women had used donor sperm, ~0.3% of reproductive-age women)
- American Society for Reproductive Medicine. Informing Offspring of Their Conception by Gamete Donation – Ethics Committee Opinion. Fertil Steril. 2018. (Recommends that children be informed of donor conception to promote healthy family dynamics and trust)
- U.S. FDA. Regulations on Donor Sperm. 21 CFR Part 1271. (Mandates infectious disease testing, quarantine of anonymous donor sperm; allows directed use of “ineligible” donor with informed consent)
